All Departments
- Anorectal Manometry
- Diagnostics Endoscopy
- Endosonography
- Esophageal Manometry
- Gastroenterology
- Sonography
- Therapeutic Endoscopy
Emergency Cases
+91 9850 077 168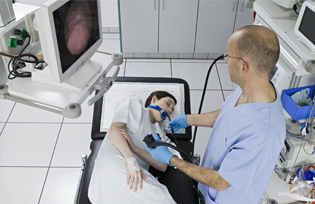
Diagnostics Endoscopy
A Diagnostic Endoscopy is an examination to look at your internal organs using an instrument called an endoscope. This is a long, tube-like instrument with a lens and light. It may be inserted through a natural opening such as the mouth or anus.
Before having an endoscope passed through the mouth, you must avoid food for several hours as food in the stomach can obstruct the consultant’s view. You are usually given laxatives before an endoscope is inserted into the rectum and colon.
More About Diagnostics Endoscopy
A diagnostic gastroscopy is usually recommended if your symptoms suggest that you have a condition that affects your upper gastrointestinal (GI) tract.
Symptoms that are often investigated using a diagnostic gastroscopy include:
- Difficulties and/or pain when swallowing (dysphagia)
- Persistent abdominal pain
- Persistent nausea and vomiting
- Unexplained weight loss
A diagnostic gastroscopy can also be used if your GP suspects that you have bleeding inside your GI tract. Persistent bleeding can significantly reduce the number of red blood cells in your body. This is known as anemia.
Symptoms of anemia include:
- Fatigue
- Breathlessness (dyspnoea)
- Pale skin
- Irregular heartbeats
In some cases, bleeding inside the GI tract can be sudden and massive, and cause symptoms such as:
- Vomiting blood – the blood can appear bright red or have a darker, grainy appearance similar to coffee granules
- Passing stools (feces) – which are very dark in color or ‘tar-like’
- A sudden, sharp pain in your abdomen (stomach) that gets steadily worse
These symptoms usually require immediate investigation with a diagnostic gastroscopy. A diagnostic gastroscopy is also used to help confirm (or rule out) the suspected diagnosis of certain GI conditions, such as those listed below:
- Peptic ulcer (also known as a stomach ulcer) – open sores that develop on the lining of your stomach.
- Gastro-oesophageal reflux disease (GORD) – is a condition where stomach acid leaks back up into the esophagus.
- Barrett’s esophagus – a condition where abnormal cells develop on the lining of the esophagus.
- Portal hypertension – is a condition where the blood pressure inside the liver is abnormally high. This leads to the development of abnormally swollen veins (varices) on the lining of the stomach and esophagus.
- For cancers of the upper GI tract, such as stomach cancer and oesophageal cancer – the endoscope can be used to remove samples of suspected cancerous tissue for testing, which is known as a biopsy.
Diagnostic gastroscopy is a non-invasive procedure, which means that it does not involve making major incisions (cuts) into the body. Therefore, it is usually suitable for most people, even if their health is not particularly good.
However, there may be a few circumstances where a diagnostic gastroscopy is not recommended. These include:
- If you have an unhealed perforation inside your GI tract
- If you have recently had a heart attack
- If you have recently had head or neck surgery (in this situation, it is usually recommended that you wait until you have fully recovered from the effects of the surgery).
Preparing for a diagnostic gastroscopy
You will usually receive written information about how to prepare for a diagnostic gastroscopy, along with your appointment letter. If there is anything that you feel needs to be clarified, call the Gastrohub hospital.
If you are referred for an endoscopy, you will need to stop taking any prescribed medicines for dyspepsia (indigestion) at least two weeks beforehand. This is because they can mask some of the problems that could show up. You can continue to take antacids up until your endoscopy.
You will be asked not to eat or drink anything for six hours before having your endoscopy. Your stomach must be empty so that the person who is performing the endoscopy can see the whole area clearly.
If you wish, you can choose to have the procedure carried out under sedation (see below) in order to help prevent food or fluid from passing into your lungs.
A diagnostic gastroscopy is not a particularly painful procedure, although some people may find it slightly uncomfortable. Therefore, you can choose the type of anesthetic that is used during the procedure:
- Local anesthetic spray is used to numb the back of your throat
- Sedation makes you very drowsy so that you have little or no awareness of the gastroscopy being carried out.
If you choose to have sedation, you will need to arrange for someone to bring you home after the procedure and to stay with you for at least 12 hours afterward.
Even if you feel very alert, the sedative can stay in your blood for around 24 hours. You may have further episodes of drowsiness during this period. Therefore, during this time, do not:
- Drive a vehicle
- Operate heavy machinery
- Drink any alcohol
If you choose to have a local anesthetic, you can leave the hospital as soon as the procedure has been completed, and you can resume your normal activities within 1-2 hours.
The procedure
A diagnostic gastroscopy is usually done at the endoscopy unit at your local hospital (although some larger GP surgeries may also offer endoscopic services).
A diagnostic gastroscopy is usually performed on an outpatient basis, which means that you will not have to stay overnight in the hospital. If, however, you choose to have a sedative and you live alone, you may have to stay in overnight.
A diagnostic gastroscopy can be performed by:
- A gastroenterologist (a specialist in disorders of the digestive tract)
- A surgeon
- An endoscopist (a doctor who has received special training in using an endoscope)
- A clinical nurse who has received specialist training in endoscopies
A nurse will talk you through the procedure to make sure that you understand why you are having it. They will ask you questions to ensure that you are properly prepared for the procedure and that you understand any associated risks. You will also be asked to sign a consent form.
At the start of the procedure, you will be asked to lie on a bed or X-ray couch, on your left-hand side. This allows the endoscopist to pass the scope more easily into your stomach. You will be given a plastic mouth guard to stop your teeth from being damaged by the endoscope as it goes down and to stop you from biting on it.
If you choose to have your gastroscopy carried out under sedation, the sedative will be injected into your arm. The medication will make you relaxed and drowsy, but you will be awake enough to follow any instructions.
If you choose to have a local anesthetic, the back of your throat may be sprayed to numb it, or you may be given an anesthetic lozenge to suck on.
Once the sedative or throat spray has worked, the doctor will put the endoscope in your mouth and you will be asked to swallow the first part of the tube. It may be a little uncomfortable to swallow, but there will be plenty of room for you to breathe around the scope and through your nose.
The doctor will gently and carefully feed the tube down into your stomach, and a short way beyond your stomach and into your intestine. You will be asked to breathe through your nose.
Once the endoscope is in your stomach, the air is blown into your stomach to allow the endoscopist to see any patches of redness, holes, lumps, blockages, or other abnormalities on a television monitor.
If any areas of abnormality are detected, a biopsy will be taken (a tissue sample from the abnormal-looking area) to send to the laboratory for closer inspection under a microscope. During the biopsy, you will not feel anything.
Once any necessary samples have been taken, the doctor will remove the endoscope by pulling it back out of your gullet and through your mouth.
After the test, you will need to rest for a while. If you have had a sedative, you may not remember much, if anything, about the test after you come around.
Results
If you have had a local anesthetic, your doctor should be able to discuss the results and implications of the gastroscopy before you leave the hospital. However, if you have had a biopsy, you will usually have to wait for seven days to get the results.
If you were sedated, you will probably still be too drowsy to understand any information. A further appointment will be made so that you can discuss the results with the doctor. Alternatively, the results of the gastroscopy may be sent to your GP.

